To schedule an mpox vaccination appointment, visit myturn.ca.gov
The CDC recently estimated a 35% likelihood of an mpox resurgence this year, based on national vaccination rates. But on Friday, May 5, the Chicago-based LGBT healthcare provider Howard Brown Health announced that seven cases of mpox had been diagnosed at their clinics since mid-April.
It’s too soon to declare a new public health emergency, but if you are at risk for mpox and have not been fully vaccinated, now is the time to do so. The best way to stop the spread of the virus is to receive both doses of the mpox vaccine. The Los Angeles County Department of Health is offering the mpox vaccine on an ongoing basis through these sites. The Los Angeles LGBT Center will be giving vaccine to our patients on an ongoing basis. Current patients can schedule a vaccination visit Mon.–Fri., 8–6 p.m. We will also be working with the Department of Health to offer the mpox vaccine at our Center South location on the second and fourth Friday of every month, 10:30 a.m.–1:30 p.m. Schedule an appointment at myturn.ca.gov.
The Los Angeles LGBT Center has been working tirelessly to respond to the human monkeypox public health crisis that is presently placing the health and safety of our community in jeopardy. We will sustain our efforts to test, treat, and vaccinate; educate; and advocate. As we know from the HIV/AIDS crisis, when the LGBTQ+ community is faced with a public health threat, we cannot rely on the government. Instead, we must take swift action.
Since human monkeypox (hMPXV*) emerged last spring as a threat to gay and bisexual men and transgender people, the Center’s team of medical providers, policy advocates, and outreach workers designed and initiated a community response plan. Our goal: combat stigma and lessen the spread through compassionate care and steadfast advocacy.
*The Center has begun using hMPXV, which is an abbreviation for human monkeypox. This abbreviation is more medically accurate and helps to reduce stigma.
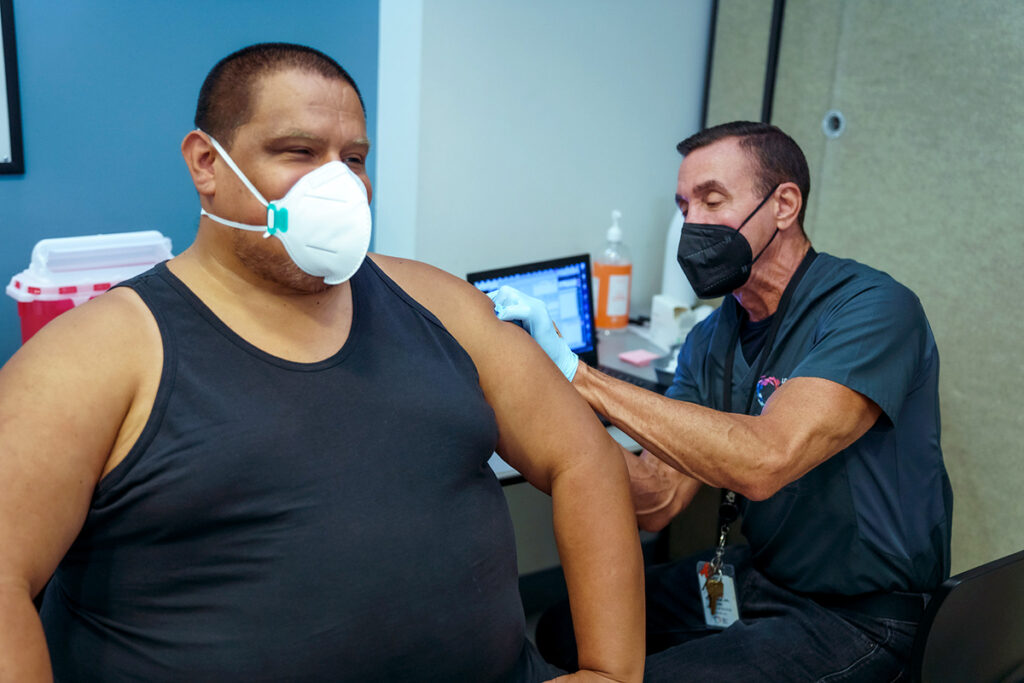

Vaccine Information
The L.A. County Department of Public Health provides the Los Angeles LGBT Center with JYNNEOS vaccine doses for human monkeypox (hMPXV). Our ability to provide vaccination is dependent on the County receiving and then distributing vaccines from the federal government. When the Center has access to vaccine doses, we are providing vaccination to existing patients who are eligible as defined by County guidance. When a Center patient becomes eligible and we have the vaccine supply necessary to provide vaccination, we will be in contact with them.
Patients of the Center who have had a known exposure to hMPXV or are showing possible symptoms are encouraged to contact their primary care provider via the patient portal or by calling the Center directly at 323-993-7500.
Individuals who are eligible but who are not established patients of the Los Angeles LGBT Center are advised to access vaccination directly from the L.A. County Department of Public Health. Information about how to access hMPXV vaccination can be found on the public health department’s website or by calling 2-1-1.
UPDATE: After a brief pause, the Center has resumed offering second doses of the JYNNEOS human monkeypox (hMPXV) vaccine, in compliance with CDC and LA DPH guidelines. Current guidance recommends two doses of Jynneos administered intradermally (into the skin), 28 days apart, for individuals at high risk1 of infection. The guidelines are based on research showing that intradermal administration of this vaccine achieves the same level of immunity while using a much lower dose. Making this change increases the available supply of vaccine by as much as five times and allows medical providers to resume offering second doses to those eligible.
It is important to remember neither one nor two doses of vaccine are 100% effective at preventing hMPXV infection. For those who believe they are at-risk for hMPXV – regardless of vaccine status – minimizing skin-to-skin contact with others by limiting sexual partners, using condoms, and wearing clothing while in crowded settings like dancefloors can help reduce the risk for transmission.
Please visit the Centers for Disease Control and Prevention’s Monkeypox Prevention site for more information.
[1] Eligibility criteria can be found here: http://publichealth.lacounty.gov/media/monkeypox/index.htm.
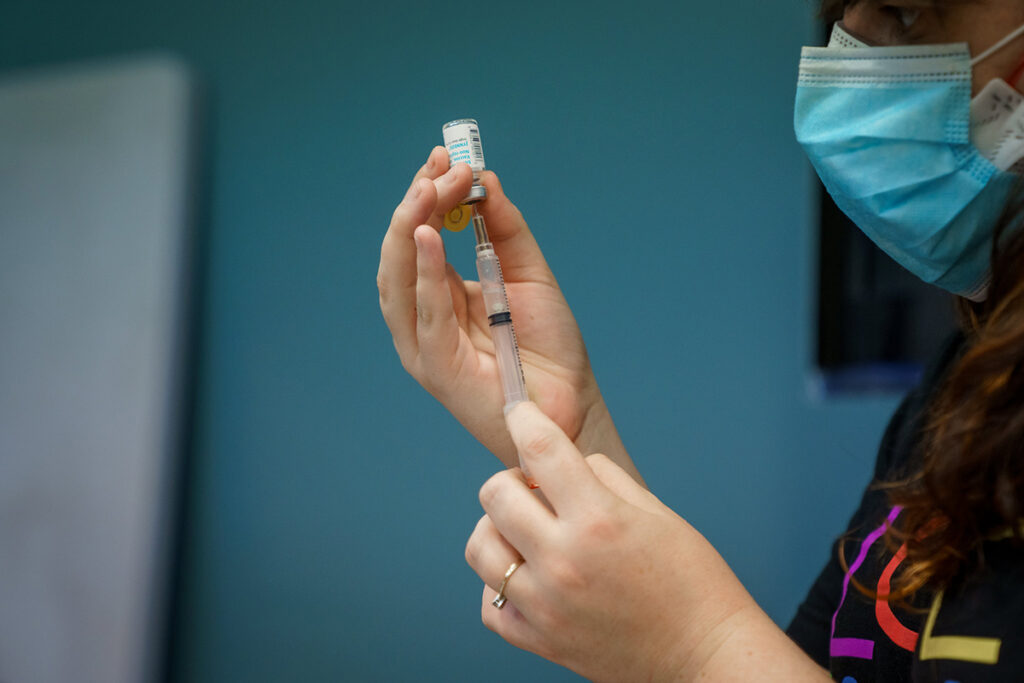
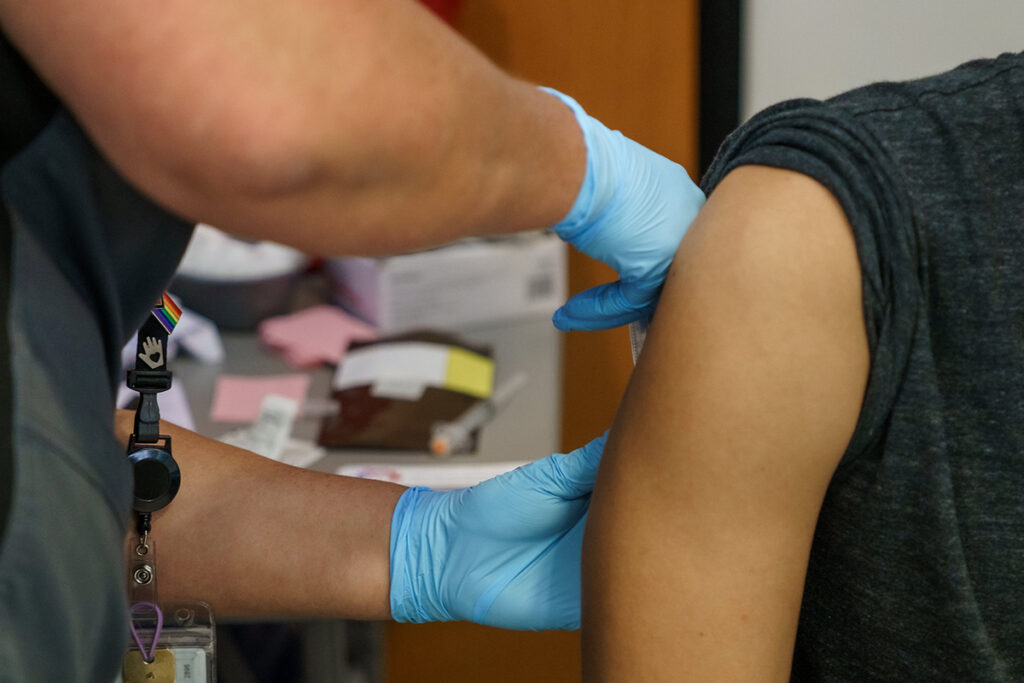
FAQ
Mpox, formerly known as the human monkeypox virus, is an infectious disease that can occur in humans and some animals.
We are still learning about mpox and transmission risk. We do know that mpox is spread mostly through prolonged skin-to-skin and face-to-face contact. Mpox virus has been found in the semen and saliva of infected individuals, but it is not clear how much this impacts transmission. The virus can also live on surfaces and fabric, though transmission risk through this route is much lower.
We learned in the 2022 outbreak that mpox presents differently in different people. Many people develop a fever or flu-like symptoms initially. A few days later, skin bumps often appear. These tend to develop at a site of recent contact with another person. The skin bumps may start as red and fat and then progress to raised and fluid filled. Eventually, the bumps fill with pus.
If you had recent prolonged skin-to-skin or face-to-face contact with someone and are now noticing flu-like symptoms or a rash, call your doctor’s office right away to discuss next steps.
For most people with mpox, supportive care and pain control is sufficient to treat mpox and the symptoms tend to resolve within 14 days.
There is a medication called tecoviramat, or Tpoxx, that has been used to treat mpox in certain situations. The medication is not FDA approved for this purpose but was made available by the FDA for this purpose under “compassionate use.” There is still limited data on the effectiveness of Tpoxx in treating mpox. The drug is recommended in mpox patients who are immunocompromised and/or experiencing severe infections. However, there may be some danger in over prescribing Tpoxx as it may increase the likelihood that the mpox virus may develop resistance to this medication.
Yes, mpox is a sexually transmitted infection. In the previous outbreak, mpox was shown to spread primarily through sexual contact. Though infections have occurred through other exposures like non-sexual contact with household members, these cases were far less prevalent. The virus also has been found in semen and saliva though we don’t have evidence that the virus can be transmitted through these fluids in the absence of lesions.
Though there is a risk of stigmatization when identifying mpox as an STI, it is important to do so because it forces us to speak explicitly about risk and prevention. Additionally, labeling the virus an STI allows us to focus our resources (both human and financial) towards the communities most at risk.
Getting two doses of the mpox vaccine is recommended for all those at risk. If possible, postpone or delay sexual activity until you are fully vaccinated. If that is not possible, talk with your partners about their vaccination status and whether or not they have any signs or symptoms of infection. Avoid touching any skin rashes or lesions on other people’s skin. Using condoms can decrease the risk of infection. However, a person may have skin lesions that cannot be covered by condoms.
Anyone who perceives themselves at risk of mpox or requests the vaccine may receive the vaccine. However, some individuals are at higher risk for mpox infection and/or more serious disease. This includes anyone who is or has been:
- Currently or planning to have sex with multiple partners
- Living with HIV and engaging sexual activity with more than one person
- Engaging in transactional sex
- Taking PrEP
- Diagnosed with an STI (like gonorrhea, chlamydia or syphilis) in the past three months
- Front-line health care and lab staff providing care to individuals at increased risk for mpox
No, if you received two doses of the mpox vaccine or if you have recovered from mpox infection, you do not need additional vaccination. The only exception are people who were immunocompromised at the time of their mpox diagnosis.
Though we are still learning about this particular virus, the assumption is that individuals who are fully vaccinated or have recovered from infection are immune. The risk of breakthrough infection is presumed to be low.
In November 2022, the World Health Organization (WHO) made the recommendation to transition the name of this virus from “monkeypox” to mpox. This was in response to stigmatizing and racist language being used to describe the origins of the virus and those at risk of infection. WHO consulted with global health experts and made the recommendation to change the name of the virus.
Based on current nationwide vaccination rates, the CDC estimates that there is a 35% chance of resurgence this summer. Additionally, the LGBT health center, Howard Brown Health in Chicago, recently diagnosed seven cases of mpox in their clinics. This news is concerning and underscores the importance of increasing vaccination rates in those at risk of infection.
Action Center
As human monkeypox cases continue to rise, we must act quickly to ensure our community can access testing, vaccines, treatment, and recovery. You can help make a difference today by sending a quick message to Secretary of Health and Human Services Xavier Becerra.
Tell the Secretary: we need action now!

Media
Center Press Releases
- Los Angeles LGBT Center Demands Biden Administration Take Further Action Following Overdue Public Health Emergency Declaration
- LGBTQ+ Organizations Call On CDC To Expand Human Monkeypox Virus Testing And Vaccine Distribution
- Los Angeles LGBT Center Applauds Gov. Newson, LA County For Declaring Human Monkeypox Health Emergency
Center Letters and Articles
Town Halls
Resources
How You Can Help
Support the Center’s human monkeypox response effort by donating now.




